Treatments keep young sickle cell patient cheering
Nyiah Young is a typical third-grader who enjoys cheerleading at school and running around with friends. Most people would not know from outside appearances that the young, active child undergoes monthly treatments for sickle cell disease and suffered a stroke at age 3.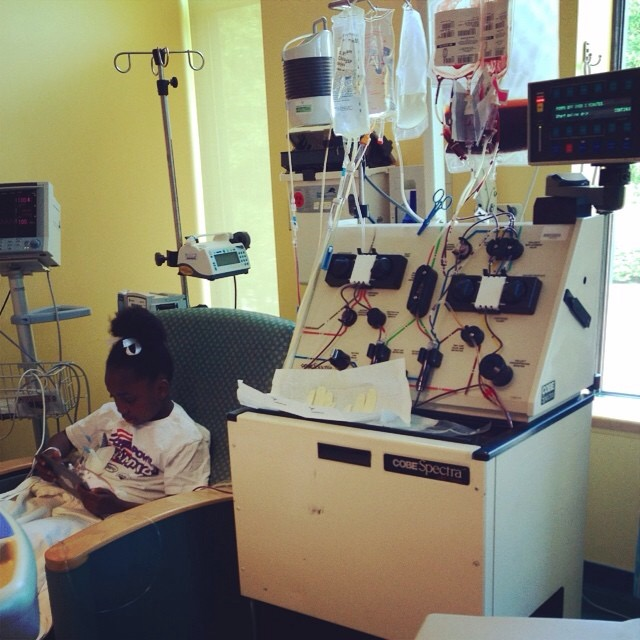
In fact, Nyiah was diagnosed with sickle cell disease, a genetic red blood cell disorder, soon after birth following routine newborn screenings. The Centers for Disease Control and Prevention estimates that sickle cell disease affects 90,000 to 100,000 Americans, and occurs in approximately one of every 500 African-American births.
The distorted shape of red blood cells in sickle cell disease can cause patients any number of complications, including painful episodes, organ damage, infections and even stroke, explains Dr. Rebecca McFall, pediatric hematologist-oncologist at Advocate Children’s Hospital in Oak Lawn, Ill.
“Stroke is the most severe complication of sickle cell,” says Dr. McFall. “Stroke occurs in roughly 10 percent of sickle cell patients. Historically, the most common burden that children with sickle cell disease face is severe bacterial infections.”
To prevent another stroke, Nyiah immediately began undergoing monthly apheresis treatments, which she continues on an ongoing basis today. Apheresis treatment, which requires a three-hour to six-hour stay in the hospital, is a transfusion that filters out a percentage of the diseased red blood cells and replaces them with normal red blood cells, explains Dr. McFall.
Apheresis treatments have proven miraculous for Nyiah. Prior to her stroke, she was hospitalized regularly for disease complications. Since starting apheresis four years ago, Nyiah has remained relatively healthy with no hospital visits,” say Carlos Young, Nyiah’s dad. “She keeps busy during the six-hour treatments by reading and finishing books.”
Although the apheresis treatments help sustain Nyiah’s health and energy levels in between the monthly hospital visits, she also undergoes treatment at home. On a daily basis, she takes penicillin, folic acid and aspirin. Carlos explains that Nyiah’s current treatment will continue until she receives a bone marrow transplant, which, oftentimes, is the only cure for blood disorder patients.
Outside the hospital, Nyiah and her family are very involved with Be the Match, an organization that encourages people to join the bone marrow registry as potential future bone marrow donors. The Young family attends fund-raising walks and community events to assist in registering people. Be the Match discovered that, on average, only about one in 500 registry members will ever match a patient and go on to donate blood marrow.
“Finding a bone marrow match can be very difficult. That’s why I encourage everyone to join the registry to potentially save the life of a sickle cell or leukemia patient,” Carlos says.
As Nyiah continues to wait for a match, she does not let the disease hinder her in any way. Instead, she has become an advocate for a cause that could help save her life, while maintaining the normal activities of an 8-year-old girl.




















Nyiah is such a brave and inspiring young girl while being active and battling this disease.
What a strong little girl. Praying she will get the bone marrow transplant she needs to live a long, healthy life.