Related Posts
Comments
2 Comments
About the Author
health enews staff is a group of experienced writers from our Advocate Health Care and Aurora Health Care sites, which also includes freelance or intern writers.
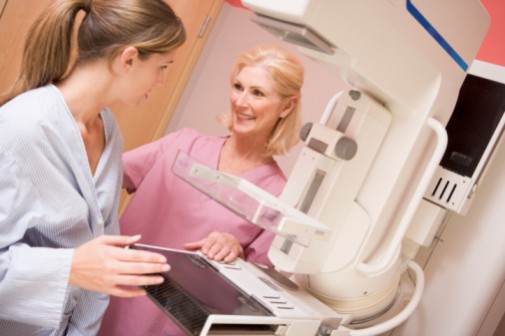
Just a few years ago, the U.S. Preventative Services Task Force, an expert panel charged with making recommendations about health practices, caused an uproar when it recommended women under age 50 did not need a screening mammogram every two years.
It was thought that the benefits of potential early detection were overshadowed by overtreatment and the anxiety over false-positive results in younger woman. However, several organizations, including the American Cancer Society, continue to hold to their recommendation that age 40 be the baseline for mammogram screening for women considered at average risk of breast cancer.
Now, a new study supports this position too. The research, performed at several Boston hospitals revealed a significant death rate in women under age 50 who did not receive regular mammograms.
The study, which was published this week in the online version of the medical journal Cancer, analyzed the medical information of more than 7,300 women diagnosed with breast cancer between 1990 and 1999, then followed until 2007.
According to the researchers, 71 percent of the 609 women who died from breast cancer had never had a mammogram, or had never undergone regular screening. And about half those who died were under the age of 50.
The researchers wrote in the study report that their findings “suggest less, or less frequent screening at ages older than 69 years, but more frequent screening for women younger than 50 years.” Breast cancer tends to be more aggressive in younger women, the authors wrote.
For many hospitals, this new information simply upholds the guidelines they’ve been following all along.
“We continue to support the American College of Radiology and American Cancer Society recommendations, starting screening mammography at the age of 40,” says Dr. Vanessa Wear, radiologist at Advocate Illinois Masonic Medical Center in Chicago. “This study confirms what we have been recommending for years—starting screening mammography at age 40 saves lives.”
Dr. Wear said the U.S. Preventative Services Task Force recommendation to start mammography at a later age may lead to more undiagnosed breast cancers.
To make getting a mammogram easier, Dr. Wear says Advocate Health Care will began offering same-day mammogram screenings for women age 40 and older without a physician referral beginning September 16.
“Early detection is key to survival,” she says. “At Advocate, we want to make sure women can get in to be screened as conveniently as possible. We believe providing this type of access empowers them to take charge of their health.”

health enews staff is a group of experienced writers from our Advocate Health Care and Aurora Health Care sites, which also includes freelance or intern writers.

With our LiveWell app and website, you can manage health and wellness for yourself and for everyone who counts on you.
Download the appGet health and wellness insights emailed to you weekly.
I am grateful to Advocate for sticking to their life saving recommendations. I am a 2x breast cancer survivor, my 1st cancer was found at the age of 44 and my second at 49. Thank You Advocate!
Tere
A look back at the history of research in favor of mammography tells you whether you should believe this new study finding or not. All pro-mammogram studies downplay or dismiss the true factual risks of mammography (Kopans, a co-author of this new study has done that again and again), practically all studies in support of mammograms are designed and implemented by people with massive conflicts-of-interests (again, Kopans, fits the bill on that one), the most influential studies in favor of mammography are severely flawed (read Rolf Hefti’s ebook “The Mammogram Myth: The Independent Investigation Of Mammography The Medical Profession Doesn’t Want You To Know About”). On top of it, a number of well-designed studies found no noteworthy reduction in mortality from breast cancer after the use of mammographic screening. Now, ask yourself, “where does this new study most likely fit in?” Mmmm… tough one, huh?